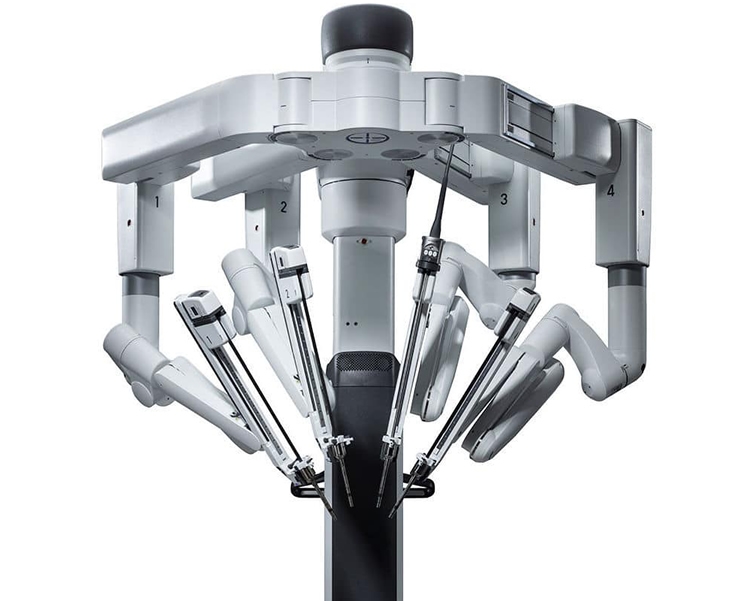
Robotic surgery offers numerous benefits, both for the patient and the surgeon. Among the main advantages are:
1. Surgical Precision: The robotic system allows for more precise and stable movements, reducing the risk of damage to surrounding tissues and increasing the effectiveness of the procedure.
2. Less Trauma to the Patient: Being minimally invasive, robotic surgery requires small incisions, resulting in less postoperative pain, less bleeding, and a lower risk of infection.
3. Faster Recovery: Patients undergoing robotic surgery usually have shorter hospital stays and return to daily activities more quickly.
4. Better Functional Outcomes: In urology, preserving sexual and urinary function is a crucial goal. The precision of robotic technology significantly contributes to better outcomes in these aspects, especially in procedures such as radical prostatectomy.
5. Comfort and Ergonomics for the Surgeon: The robotic platform offers doctors a more comfortable working position, reducing fatigue and allowing greater focus during long surgeries.
6. Advanced Visualization: High-definition cameras and three-dimensional vision provide the surgeon with an enlarged and detailed view of the operated area, facilitating the identification of delicate structures.